We offer medical detox and multiple addiction treatment options in our
luxury treatment centres in Port Hope, Cobourg, and Ottawa.
What are the causes of Alcoholic Hepatitis?
Alcoholic hepatitis is an inflammatory liver condition triggered by excessive drinking over months or years. Your liver handles the hard work of metabolizing every drink you consume, but there's a limit to what it can handle. Push past that limit repeatedly, and the organ starts fighting back with swelling, scarring, and cell death. At the Canadian Centre for Addictions, we see firsthand how chronic alcohol use quietly erodes liver function long before any symptoms show up, and why catching these warning signs early makes all the difference.
Key Takeaways:
- How a single toxic byproduct of alcohol metabolism, not alcohol itself, does the real damage to your liver cells, and why your body can lose over 70% of liver function before a single blood test raises a flag.
- Why only 35% of heavy drinkers develop this condition, and which six risk factors determine whether you're in that group.
- The two-way relationship between alcohol dependence and liver damage – and what recent Canadian pandemic data reveals about who's being hit hardest.
- How much time do you actually have to reverse alcohol-related hepatitis before scarring becomes permanent, and what does the 10% recovery stat really mean.
- The specific warning signs that warrant medical evaluation now, not next month.
How Does Chronic Alcohol Use Damage Your Liver?
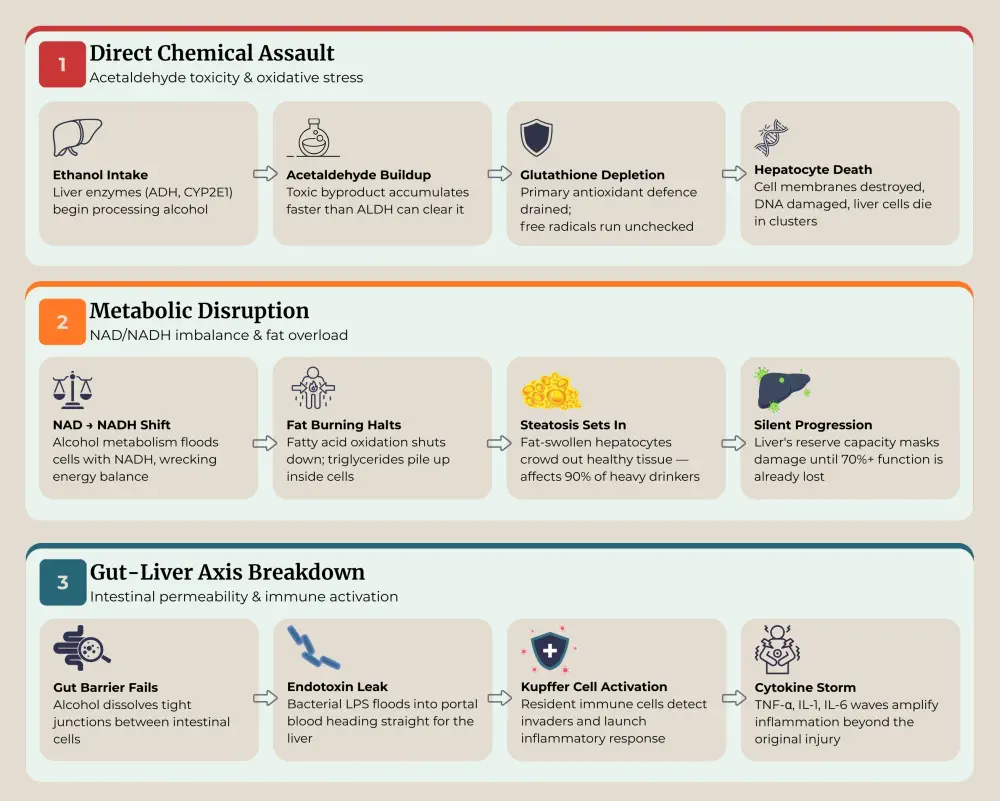
Your liver metabolizes alcohol through enzyme systems that convert ethanol into acetaldehyde, a substance far more toxic than alcohol itself. Chronic alcohol use overwhelms these enzymes, and acetaldehyde accumulates faster than your body can neutralize it. Direct chemical damage to hepatocytes (liver cells), membrane destruction, and depletion of glutathione, your liver's primary antioxidant defence.
Alcohol metabolism also alters your liver's internal chemistry by converting NAD to NADH. This disrupts fatty acid oxidation, causing fat to pile up inside hepatocytes – a condition called steatosis. About 90% of heavy drinkers end up with fatty liver. The organ's massive functional reserve masks the problem: your liver can lose over 70% of its working capacity before blood tests flag anything abnormal, which is why routine lab panels miss early alcohol-related damage.

Heavy drinking also damages the gut lining. Alcohol weakens the tight junctions between intestinal cells, allowing bacteria and bacterial toxins (lipopolysaccharides) to leak into portal blood flowing toward the liver. These bacterial products activate immune cells called Kupffer cells, which unleash waves of inflammatory cytokines(TNF-alpha, interleukin-1, interleukin-6) that amplify liver inflammation and accelerate cell death. This gut-liver axis disruption explains why damage to the liver can worsen faster than drinking habits alone would predict.

Who Faces the Highest Risk of Alcoholic Hepatitis?
Not every heavy drinker gets alcohol-related hepatitis. Only about 35% of people with prolonged, excessive alcohol intake end up with the condition, which tells us that other forces shape individual vulnerability. Several well-documented risk multipliers determine who crosses that threshold and who doesn't.

A population-based study from Queen's University published in JAMA found that alcohol-associated hepatitis (AH) cases among young adults, particularly women, have surged over the past two decades in Ontario. Women showed a 50% higher risk of reaching cirrhosis compared to men, and 37% of female survivors had progressed to cirrhosis or decompensation at a median follow-up of four years after their first episode.
How Does Alcohol Addiction Drive Liver Disease?
Alcohol addiction creates the exact drinking behaviours that produce sustained liver damage. Casual drinkers rarely hit the thresholds associated with AH. Most diagnosed patients report consuming upwards of 100 grams of alcohol daily for a decade or longer. That volume of intake rarely happens without dependency driving it.
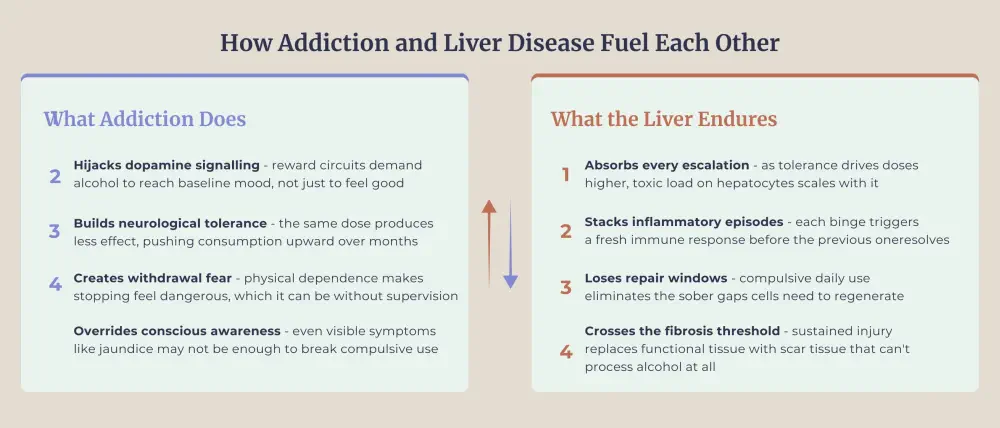
Chronic, heavy alcohol consumption rewires brain reward circuits, making it harder to stop drinking even when physical consequences become obvious. The liver accumulates damage silently through repeated inflammatory episodes. By the time jaundice, abdominal pain, or unexplained fatigue appear, the disease has been worsening for years.
Canadian data tells a grim story. A study found that alcohol-related liver disease deaths rose 22% during the COVID-19 pandemic, with ALD hospitalizations climbing 23%, the largest relative increase of any alcohol-attributable condition. Adults aged 25–44 saw the steepest mortality spikes at 55%. These numbers capture what happens when stress, isolation, and reduced access to support systems collide with alcohol dependence.
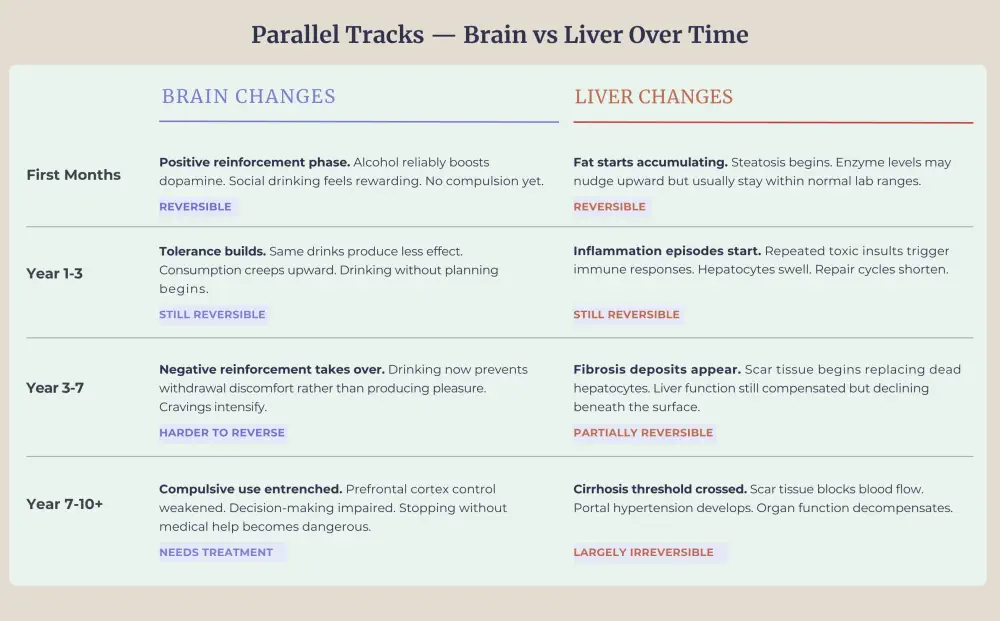
Can You Reverse Alcoholic Hepatitis Before Permanent Liver Damage Sets In?
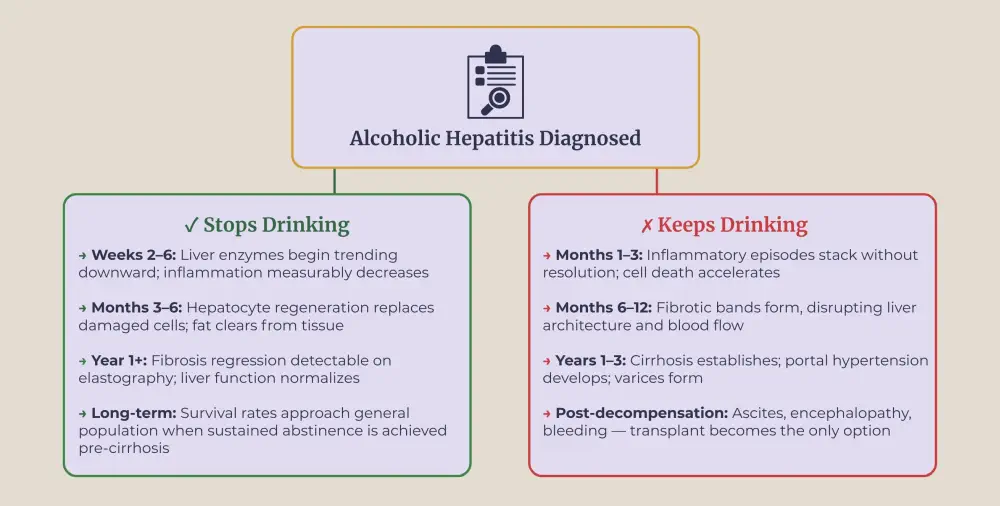
Yes, but timing matters enormously. Mild alcohol-related hepatitis can resolve completely once a person stops drinking. The liver has impressive regenerative capacity when given the chance to recover. About 10% of patients who achieve full alcohol cessation return to normal liver histology on follow-up biopsies.
The window closes quickly, though. Continued drinking pushes mild inflammation toward fibrosis and then cirrhosis, permanent scarring that blocks blood flow and cripples liver function. Roughly 70% of people with this condition who keep drinking reach cirrhosis. Once that scarring sets in, the damage becomes largely irreversible, and median survival without transplantation drops to about two years after decompensation.
Quitting alcohol abruptly after heavy, prolonged use carries its own dangers. Withdrawal can trigger seizures, delirium tremens, and severe blood pressure instability. Medically supervised detox provides the safest pathway, managing withdrawal symptoms and protecting already-stressed organs from additional harm.

Is Your Drinking Pattern Putting Your Liver at Risk?
Persistent upper-right abdominal discomfort, unexplained nausea, yellowing skin or eyes, dark urine, and unusual fatigue all warrant medical evaluation, especially if you've been drinking heavily. Don't wait for multiple symptoms to appear. Liver inflammation can produce subtle signals that are easy to dismiss as stress or poor sleep.
If you recognize signs of alcohol addiction in yourself or someone close to you, the Canadian Centre for Addictions offers physician-monitored detox, individual counselling, and long-term recovery support at our facilities in Port Hope and Cobourg, Ontario. We treat the whole person, addressing the dependency that causes ongoing liver damage alongside the physical and emotional toll of addiction.
Recovery starts with one conversation. Contact the Canadian Centre for Addictions at 1-855-499-9446 to discuss your needs with our experienced team. We'll help you take the steps that protect your liver and rebuild your health.
FAQ
How much alcohol causes alcoholic hepatitis?
Most diagnosed patients consumed over 100 grams daily (roughly seven standard Canadian drinks) for a decade or more. But women, people with hepatitis C, and those carrying excess weight can reach the same damage at lower volumes. Binge patterns raise risk, too. Heavy sessions create sharper oxidative spikes than the same weekly total spread across seven days.
Can you get alcoholic hepatitis from binge drinking?
Yes. Rapid blood alcohol spikes produce more severe oxidative stress and inflammation than the same volume consumed gradually. Repeated binge episodes over months or years can trigger alcohol-related hepatitis even without daily drinking, particularly in younger adults.
Is alcoholic hepatitis the same as cirrhosis?
No. AH is active liver inflammation that can still be reversed if drinking stops. Cirrhosis is permanent scar tissue replacing functional cells, largely irreversible. The two conditions can co-exist, and doctors distinguish them through different markers: hepatitis shows an AST-to-ALT ratio above 2:1, and cirrhosis requires imaging or biopsy to confirm scarring.
How long does it take for alcoholic hepatitis to come on?
Most patients present after 10 or more years of heavy drinking, typically between ages 40 and 60. Cases have been documented after as few as three months of extreme intake. Shorter timelines are increasingly common among younger adults, particularly women, who sustain liver injury from lower alcohol volumes than men.
Can addiction treatment help prevent alcoholic hepatitis?
Yes. Medically supervised programs address the dependency driving liver-damaging consumption. Patients who achieve sustained sobriety before cirrhosis sets in give hepatocytes a real chance to repair and regenerate. Structured programs also correct nutritional deficiencies that impair liver healing and reduce the relapse risk that would restart the cycle.
What are the early warning signs of alcoholic hepatitis?
Yellowing of the skin or eyes (jaundice), persistent upper-right abdominal pain, unexplained nausea, dark urine, and unusual fatigue. Fever and rapid weight loss can also appear. These symptoms often get dismissed as stress or a poor diet. If you've been drinking heavily and notice any combination, get a medical evaluation promptly.
Can you survive severe alcoholic hepatitis?
Severe cases carry a 30-day mortality rate between 30% and 50%, depending on how advanced the inflammation is at diagnosis. Survival improves dramatically with immediate alcohol cessation, corticosteroid treatment where appropriate, and nutritional support. Patients who stop drinking and complete structured recovery programs have significantly better long-term outcomes than those who continue.
Article sources
- Singal, A.K., & Mathurin, P. (2021). "Diagnosis and Treatment of Alcohol-Associated Liver Disease: A Review." JAMA, 326(2), 165–176. Available at: https://pubmed.ncbi.nlm.nih.gov/34255003/
- Gao, B., & Bataller, R. (2011). "Alcoholic Liver Disease: Pathogenesis and New Therapeutic Targets." Gastroenterology, 141(5), 1572–1585. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3214974/
- Flemming, J.A., et al. (2024). "Epidemiology and Outcomes of Alcohol-Associated Hepatitis in Adolescents and Young Adults." JAMA Network Open, 7(12), e2452459. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11681377/
- Shi, Y., et al. (2025). "Mortality and hospitalizations fully attributable to alcohol use before versus during the COVID-19 pandemic in Canada." CMAJ, 197(4), E87–E95. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11790301/
- Jophlin, L.L., et al. (2024). "ACG Clinical Guideline: Alcohol-Associated Liver Disease." American Journal of Gastroenterology, 119(1), 30–54. Available at: https://pubmed.ncbi.nlm.nih.gov/38174913/
- Mackowiak, B., et al. (2024). "Alcohol-associated liver disease." Journal of Clinical Investigation, 134(3), e176345. Available at: https://www.jci.org/articles/view/176345






