We offer medical detox and multiple addiction treatment options in our
luxury treatment centres in Port Hope, Cobourg, and Ottawa.
Do Edibles for Sleep Really Work and What Are the Risks?
Cannabis-infused gummies have become one of Canada's most popular bedtime rituals, with millions reaching for edibles for sleep as an alternative to prescription pills. The marketing logic is seductive – no smoke, no pharmacy counter, just a familiar-looking candy before bed. But repackaging a psychoactive drug as a wellness product doesn't change what it does inside the brain. Cannabis for sleep divides scientific opinion – short-term aid for some, quiet erosion of sleep quality for others, and the addiction risk that sits beneath both outcomes rarely makes it onto the label.
Key takeaways:
- Why edibles feel different from other sleep aids – and why the reason they feel safer is the same reason they warrant more scrutiny, not less.
- What THC is doing to your brain while you sleep – including one change that begins quietly, long before any obvious symptoms appear.
- Who the research says benefits from cannabis for sleep – and what the data shows happens to everyone else who uses it for the same purpose.
- How a single nightly gummy can become two, and why stopping is harder than starting – including how long the disruption lasts once you try to quit.
- Which three groups absorb the dependency risk fastest – and why, for each of them, the biological reason is entirely different.
What Are Edibles for Sleep, and Why Are So Many Canadians Using Them?
Edibles for sleep are cannabis-infused food products (gummies, chocolates, beverages, and capsules) taken at bedtime to reduce the time it takes to fall asleep or ease nighttime waking. Unlike smoking or vaping, they pass through the digestive system before entering the bloodstream, which delays onset but stretches duration considerably.
The appeal is straightforward. Over-the-counter sleep aids cause next-day sedation. Prescription medications carry dependence concerns. Cannabis, now legal across Canada, carries a health-food-store glow that neither of those does. Edibles are discreet, palatable, and predictably dosed. None of that makes THC something other than a psychoactive drug, one with documented addiction potential that Health Canada recognizes as cannabis use disorder. "Natural" and "non-addictive" are not synonyms. The science makes that distinction sharply.
What Happens When You Sleep High on an Edible?
Going to bed high on an edible is a different experience from smoking before sleep. The digestion route changes everything. Onset arrives anywhere from half an hour to ninety minutes later, and effects can linger for up to eight hours. That extended window aligns with a full sleep cycle on paper, but overshooting the dose or misjudging timing leaves you foggy well into the next morning.
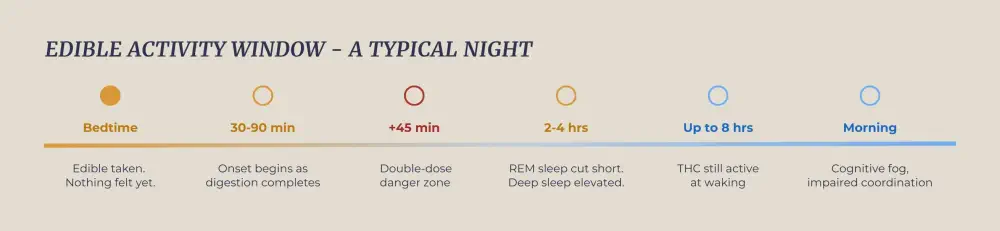
Inside the brain, THC engages the endocannabinoid system in ways that measurably alter sleep architecture. Research published in PMC shows that acute THC use shortens sleep onset and may increase deep slow-wave sleep initially, the most physically restorative stage. The trade-off is REM sleep. THC tends to suppress rapid eye movement (REM) sleep, the stage during which the brain files memories, processes emotions, and generates dreams. A 2025 systematic review and meta-analysis confirmed that withdrawal from regular use reliably triggers REM rebound – intense, deeply disturbing dreams that surge back once cannabis stops. Fewer dreams during active use, vivid, distressing ones when you quit.
What most people using edibles for sleep don't register is that this same endocannabinoid system begins downregulating its own natural activity in response to repeated THC exposure. The brain, reading THC as a substitute for its own signalling molecules, reduces production of them. That's not a side effect. That's the neurological beginning of dependency, the point at which the body starts requiring the drug to reach states it used to reach on its own.

Edibles also carry a specific risk of over-ingestion. Because the onset is slow, users who don't feel effects within 45 minutes frequently take a second dose (only to have both arrive simultaneously). High-dose THC can trigger severe anxiety, racing heart, nausea, and disorientation, none of which contribute to a restful night.
Do Edibles Work for Sleep?
Cannabis for sleep produces real, measurable effects for some people, and that's precisely what makes it dangerous to treat casually. A drug that reliably delivers relief is a drug with reliable addiction potential.

Studies of people with chronic pain and anxiety-related sleep problems show the most consistent benefits. A 2022 retrospective chart review by Vaillancourt et al. found that 71% of insomnia and sleep disorder patients at an Ottawa medical cannabis pharmacy reported subjective sleep improvement, and 39% were able to reduce or discontinue their prescription sleep medications entirely. For these groups, cannabinoids address the underlying barrier, pain or hyperarousal, without forcing sedation directly.
For people without those conditions, results are far more mixed. PMC research found frequent edible use was associated with shorter sleep duration, worse sleep efficiency, and lower overall sleep quality scores. Edible users also spent more time awake in bed after initially falling asleep, a fragmentation pattern that undercuts the original goal.
There's also a meaningful gap between how users perceive their sleep and what objective measurements show. Feeling deeply rested isn't always the same as sleeping well. And feeling like you can't sleep without an edible isn't a preference – it's a warning sign.

What Are the Edibles Side Effects?
Edibles side effects span a wider range than most first-time users anticipate.

Nightly use introduces a predictable escalation pattern. Tolerance climbs steadily, driving dose increases. What began as half a gummy becomes a full one, then two. Psychological dependence follows; reliance on edibles to initiate sleep becomes a problem in its own right. This isn't a personality trait or a lack of discipline. The brain has physically reorganized itself in response to the drug's presence.
Cannabis use disorder is a formal diagnosis in the DSM-5. It applies when someone continues using cannabis even as negative consequences accumulate – disrupted sleep, impaired next-day function, failed attempts to stop. The gummy shape, the legal dispensary, the wellness branding: none of it changes the pharmacology. THC is a psychoactive substance. Repeated nightly exposure to any psychoactive substance carries addiction risk, and edibles are no exception.
Stopping suddenly triggers its own consequences. Research found that among heavy cannabis users, sleep disturbances tend to begin within 24–72 hours of stopping use and, crucially, worsen over subsequent nights, not improve. These disruptions can persist for up to six to seven weeks.

That extended withdrawal window means the insomnia that returns when someone stops edibles can feel worse than the original sleep problem, which makes quitting far harder than most people expect.
Drug interactions also deserve attention. CBD, present in many sleep edibles, competes for the same liver enzymes that metabolize numerous common medications, potentially altering how long those drugs stay active in the body. Anyone on regular prescriptions should consult a physician before adding cannabis to their nighttime routine.
Who Should Be Most Cautious About Cannabis for Sleep?
CBD drug interactions are just one layer of the risk picture. Certain groups carry far greater exposure to the downsides, and for them, the calculus changes considerably.

People in recovery from any substance use disorder should treat edibles with particular caution, and the "natural" framing makes them especially dangerous for that group. A person who spent years fighting dependence on alcohol or opioids may genuinely believe a legal cannabis gummy sits in a different category. It doesn't. Regular cannabis use can graduate into cannabis use disorder. For those whose brain reward circuitry has already been sensitized by prior substance exposure, that progression can happen faster and with less warning than it would in someone with no history. At the Canadian Centre for Addictions, we see this dynamic regularly. A patient begins using edibles to manage withdrawal-related insomnia; the relief they provide becomes a reliance of its own. Addressing both the sleep problem and the substance concern together is the most reliable path forward.

Young people under 25 face an elevated risk, too. The adolescent brain is still forming its reward and impulse-control circuitry, regions that cannabis directly affects through the endocannabinoid system. Starting regular use during this window raises the lifetime risk of cannabis use disorder considerably; research consistently shows that earlier onset of use predicts higher rates of dependence in adulthood. Older adults sit at the opposite end of the dosing problem. THC is metabolized more slowly with age, meaning standard doses hit harder and last longer than younger users experience, increasing fall risk during nighttime bathroom trips.
What Happens When Relief Becomes a Requirement?
A gummy bear is still a drug delivery system. That sentence shouldn't need saying, but the normalization of edibles for sleep in Canadian culture has made it necessary. When a substance is sold in a candy shape at a retail store, the psychological distance from "taking medication" collapses, and so does the instinct to monitor dependency.
Cannabis use disorder is real, recognized, and more common than most edibles users believe. A 2024 review co-authored by researchers at CAMH found that approximately one in five regular cannabis users will meet the clinical criteria for cannabis use disorder, and among those who use daily, that figure climbs to roughly one in three. Nightly bedtime use – consistent, habitual, relief-seeking, sits precisely in the behavioural pattern that raises that risk. The brain doesn't receive different signals because the dose came in a gummy. THC is THC. The reward pathway doesn't read the packaging.
This doesn't mean sleep problems should go unaddressed. It means they deserve a response that doesn't quietly trade one dependency for another. The Canadian Centre for Addictions offers confidential assessment and treatment for anyone concerned about their cannabis use, its effect on their sleep, or the role it may be playing in their recovery. Call us at 1-855-499-9446.
FAQ
Are edibles better than smoking cannabis for sleep?
Edibles eliminate the respiratory risks that come with smoking, but they carry distinct concerns. Delayed onset raises the risk of taking too much, effects last far longer than inhaled cannabis, and high-dose reactions can be more intense and harder to ride out.
What happens when you sleep high every night?
Nightly use leads to tolerance, meaning the same dose becomes progressively less effective. Research links habitual use to poorer sleep efficiency, reduced REM sleep, and more time spent awake in bed, exactly the reverse of what users originally sought.
How long do edibles for sleep take to kick in?
Expect 30–90 minutes on average, though a full stomach can extend that to two hours. Avoid taking a second dose because the first feels slow; both will arrive, and the combined effect can be overwhelming.
Can cannabis for sleep cause dependence?
Yes. Regular reliance on edibles to fall asleep is a recognized form of psychological dependence. Stopping abruptly can trigger rebound insomnia, anxiety, irritability, and vivid dreaming for several weeks. Tapering gradually reduces the severity of these effects.
When should I seek help for cannabis use and sleep problems?
If you can't fall asleep without edibles, find yourself increasing the dose to get the same effect, or have tried cutting back and struggled, those are signs worth taking seriously. A healthcare provider or addiction specialist can help separate sleep difficulties from cannabis dependence and address both effectively.
Article sources
- Velzeboer R, et al. (2025). "Cannabis and sleep architecture: A systematic review and meta-analysis." Sleep Medicine Reviews. Available at: https://pubmed.ncbi.nlm.nih.gov/40967124/
- Bhagavan C, et al. (2021). "Effects of Cannabinoids on Sleep and their Therapeutic Potential for Sleep Disorders." Neurotherapeutics. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8116407/
- Winiger EA, et al. (2021). "Cannabis Use and Sleep: Expectations, Outcomes, and the Role of Age." Addictive Behaviors. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC7572650/
- Vaillancourt R, et al. (2022). "Cannabis Use in Patients with Insomnia and Sleep Disorders: Retrospective Chart Review." Canadian Pharmacists Journal. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC9067069/
- Bolla KI, et al. (2008). "Sleep Disturbance in Heavy Marijuana Users." Sleep. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC2442418/
- Le Foll B, et al. (2024). "Cannabis Use Disorder: From Neurobiology to Treatment." Journal of Clinical Investigation. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11473150/






