We offer medical detox and multiple addiction treatment options in our
luxury treatment centres in Port Hope, Cobourg, and Ottawa.
Is Gabapentin Addictive? Symptoms and Treatment
Gabapentin was once dismissed as a low-risk medication, an anticonvulsant that doctors felt comfortable prescribing broadly, confident it wouldn't cause the problems associated with opioids or benzodiazepines. The clinical record tells a different story now. Gabapentin abuse has risen sharply across North America, and Canada is no exception. What began as a neuropathic pain medication and seizure treatment has become one of the most misused prescription drugs in addiction treatment settings, largely undetected, because it rarely shows up on standard drug screens.

Prescribed under brand names like Neurontin, Gralise, and Horizant, gabapentin had approximately 3.9 million prescriptions filled in Canada in 2015 alone. The drug produces feelings of calm and, at high doses, euphoria. For people with a history of substance use, that combination is a serious red flag, one that clinicians and families need to take seriously before dependency takes hold.
Key Takeaways:
- Why gabapentin addiction is so easy to miss – and the specific behavioural signs that separate genuine dependency from someone following their prescription.
- What makes gabapentin habit-forming for certain people but not others, including the role poly-substance use plays in pushing risk to a genuinely dangerous level.
- Which gabapentin side effects are manageable at therapeutic doses – and which ones become medically serious depending on what else is in the picture.
- Why gabapentin withdrawal catches people off guard, including a seizure risk that most patients and some clinicians don't see coming.
- What treatment looks like for a dependency with no approved pharmacological substitute, and why that makes professional support non-negotiable.
What Are the Signs and Symptoms of Gabapentin Addiction?
Recognising gabapentin abuse is harder than spotting dependency on more stigmatised substances. The drug is legal, widely prescribed, and consistently overlooked during drug screening. Someone in the middle of a dependency may appear to be doing exactly what their doctor ordered.
Behavioural Warning Signs
The behavioural and physical signs are recognisable to anyone paying attention.
Taking doses higher than prescribed is one of the earliest indicators, rationalised as managing uncontrolled pain or anxiety. Visiting multiple doctors to obtain separate prescriptions (a pattern called "doctor shopping") signals that the person is seeking more than therapeutic relief.
Physical Changes That Signal a Problem
Physical changes can include unusual sedation, slurred speech, poor coordination, and memory lapses. These symptoms are particularly concerning when they appear inconsistently, suggesting the person is dosing unpredictably or combining gabapentin with other substances. Running out of prescriptions early, preoccupation with the next dose, and irritability when access is disrupted are further warning signs.
Psychological and Social Deterioration
On a psychological level, people dependent on gabapentin may withdraw socially, lose interest in activities they previously valued, or show difficulty maintaining responsibilities at work or at home. Cravings are real, and distinct from simply wanting pain relief. The drug's calming, sometimes euphoric properties at elevated doses create the same hunger for repetition that defines dependency across all substances.

Why Can Gabapentin Be Addictive?
Gabapentin's addiction potential is real, though it operates differently from opioids or stimulants. At therapeutic doses, the drug inhibits calcium channels in the brain, reducing excitatory nerve activity. Push the dose higher, many people who misuse gabapentin take 3,000 mg to 8,000 mg daily, compared to the therapeutic ceiling of 3,600 mg, and the drug produces sedation, relaxation, and in some users, a marijuana-like euphoria. That reward is the hook.
Physical dependence takes hold when the brain adapts to gabapentin's presence and begins relying on it to maintain equilibrium. Tolerance sets in when the same dose stops producing the same effect, pushing the person to take more. What started as managing nerve pain or insomnia becomes a compulsion that resists stopping.
The Role of Poly-Substance Use
Gabapentin abuse is rarely an isolated behaviour. Research consistently shows that dependency takes root most readily in people who are also using opioids, alcohol, benzodiazepines, or other central nervous system depressants. Gabapentin amplifies the high of opioids, making it attractive to people seeking more from smaller quantities of harder drugs. It has also been used to blunt cocaine withdrawal, manage opioid cravings, and intensify the sedating effects of alcohol.

This poly-substance pattern carries grave consequences. A population-based study of Ontario opioid users found that co-prescription of gabapentin raised the odds of opioid-related death by 49% overall, and by approximately 60% at moderate-to-high doses. When layered on top of alcohol or benzodiazepines, the CNS suppression is additive: breathing slows, consciousness dims, and overdose risk climbs steeply. In one US toxicology analysis, 85–90% of overdose deaths where gabapentin was detected also involved opioids.
Why the Dependency Trap Catches People Who Never Sought a High
What makes gabapentin dependency clinically distinct is that a large portion of those who become dependent never misused the drug at all. Someone prescribed gabapentin for postherpetic neuralgia, diabetic neuropathy, or chronic back pain may take the medication exactly as directed for months, then find that stopping it is not straightforward. Physical dependence can take hold at therapeutic doses with consistent use – no escalation required. These patients had no intention of misusing anything. They simply followed a prescription.
This separates gabapentin from drugs where dependency is driven primarily by the euphoric reward. Research estimated that 15–22% of people with opioid use disorder also misuse gabapentin, which captures the recreational pattern. But alongside that population sits a much larger, less visible group: patients who became dependent through legitimate treatment and have no addiction history at all.

Both groups face the same withdrawal syndrome. Both groups need the same careful tapering. The drug makes no clinical distinction between them.
Side Effects of Gabapentin Use
Gabapentin side effects divide broadly into those that appear at therapeutic doses and those that emerge with misuse or high-dose use.
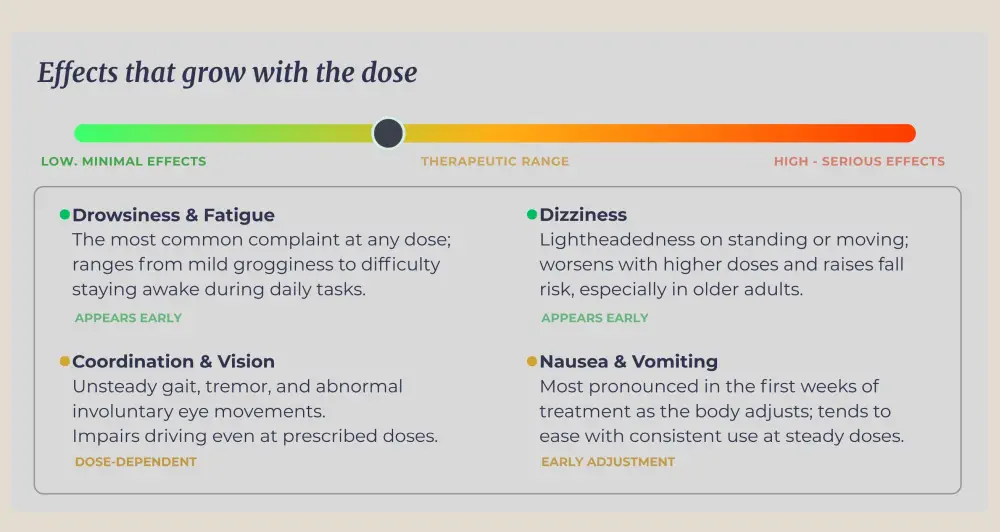
At standard doses, drowsiness and dizziness are the most common complaints. Coordination problems, unusual eye movements, and fatigue are also frequently reported. These effects are dose-dependent. They worsen as the amount taken increases. Nausea and vomiting occur particularly during the early period of use, as the body adjusts to the medication.
More concerning are the psychological gabapentin side effects. Mood changes, depression, and anxiety can appear during use and become markedly worse during discontinuation. The prescribing information for Neurontin carries an explicit warning about suicidal thoughts and behaviour. A risk that applies to anyone taking anticonvulsant medications, not only those with epilepsy. Young people appear especially vulnerable to these mood shifts.
Respiratory depression deserves particular attention. On its own, gabapentin rarely suppresses breathing to a dangerous degree. Taken alongside opioids, sedatives, or alcohol, that calculus changes dramatically. People over 65 and those with pre-existing lung conditions such as COPD face the greatest risk of serious breathing complications. For anyone comparing hydroxyzine vs gabapentin for sleep as a management option, knowing these risks before combining anything is non-negotiable.
These side effects emerge during active use. What happens when someone tries to stop is a separate, and in many ways more dangerous, medical reality.
Gabapentin Withdrawal
Gabapentin withdrawal is frequently underestimated, and that gap in awareness has led to real harm. The syndrome generally sets in within 12 hours to 7 days after the last dose, though the timeline varies based on how much a person was taking, how long they used it, and if other substances are involved.

Symptoms commonly persist for 5 to 10 days, and in some people, anxiety, sleep disturbance, and mood instability stretch to several weeks or longer.
The physical symptoms of quitting gabapentin (profuse sweating, heart palpitations, nausea, restlessness, and muscle pain) are severe enough to drive most people back to using. Insomnia and heightened anxiety are the psychological symptoms that tend to linger longest, making early recovery particularly fragile.
The Seizure Risk
Perhaps the most urgent clinical concern is seizure. Abrupt discontinuation of gabapentin can trigger epileptic seizures, including status epilepticus – a continuous, uncontrolled seizure state that constitutes a medical emergency. What makes this particularly alarming is that it can happen in people with no prior history of epilepsy or seizure disorder. A case published in PubMed documented a 34-year-old man with no seizure history who developed status epilepticus two days after running out of gabapentin, which he had been taking for chronic back pain at high doses. The medical evaluation found no alternative cause.
The Neurontin prescribing information confirms postmarketing reports of seizures following discontinuation, alongside depression and suicidal ideation. For people who have been taking gabapentin at high doses, or those tapering from poly-substance use, the seizure risk is not a remote possibility; it demands active medical planning and monitoring.
Why Supervised Detox Is the Only Safe Option
Stopping gabapentin independently, even with good intentions and a gradual plan, is not advisable for anyone with established physical dependence. The unpredictability of gabapentin withdrawal means that symptoms can escalate faster than a person at home can manage. Seizures can occur without warning. Severe anxiety can drive relapse within hours.

Medical detox in a supervised clinical setting provides the infrastructure for safe discontinuation. Healthcare teams use slow dose reduction protocols, no more than 300 mg every two to three days, adjusted based on how the person is responding. Heart rate, blood pressure, and oxygen levels are monitored continuously. Medications to manage anxiety, nausea, insomnia, and seizure risk are available immediately if needed. For those coming off gabapentin alongside opioids or other substances, this level of oversight becomes even more critical because the interactions between withdrawal syndromes can compound unexpectedly.
Treatment for Gabapentin Addiction
Gabapentin dependency presents a treatment challenge that distinguishes it from most other prescription drug dependencies: there is no approved pharmacological substitute. With opioid dependency, medication-assisted treatment, such as methadone or buprenorphine, bridges the gap between active use and sustained recovery by addressing the same receptor systems. No equivalent exists for gabapentin. Treatment teams must manage the withdrawal and simultaneously address whatever underlying condition the drug was treating (nerve pain, anxiety, seizures, or insomnia) without reaching for the same drug class.
The Dual Demand
That dual demand is where most unsupported taper attempts fail. A person who stops gabapentin without alternatives for their original pain or sleep condition will experience the return of those symptoms, stacked on top of withdrawal. Distinguishing between what is withdrawal and what is the resurgence of an underlying condition requires medical assessment, which is one reason home detox rarely succeeds.
Evidence-Based Treatment
Following medical detox, evidence-based treatment addresses the psychological layers. Individual therapy examines the patterns that reinforced use. Group counselling provides accountability and peer support from people navigating the same recovery pressures. Concrete relapse prevention planning accounts for the original medical need, because that need doesn't disappear with the dependency. At the Canadian Centre for Addictions, our facilities in Port Hope and Cobourg offer residential treatment in a private, supportive setting, with three physicians on staff and a 95.6% success rate across our programmes.

Long-Term Support After Discharge
Aftercare matters beyond discharge. Lifetime aftercare support means the risk of relapse into gabapentin abuse or other substances stays under consistent review over time, not just for the weeks immediately following treatment.
Call us today at 1-855-499-9446 to speak with our team about treatment options.
How Much Longer Can Gabapentin Dependency Stay Hidden?
Gabapentin's reputation as a benign alternative to opioids was always somewhat optimistic. The evidence now shows it carries real dependency risk – one that intensifies with high-dose use, poly-substance combinations, and a personal history of substance use disorders. Stopping Gabapentin can be genuinely dangerous, and the seizure risk alone makes unsupervised discontinuation a gamble no one should take.
What makes the situation more difficult to address is a regulatory gap that allows the problem to stay undercounted. Gabapentin remains unscheduled federally in Canada, and most provinces lack mandatory prescription drug monitoring programme requirements for it. That means dispensing data is incomplete, and misuse goes untracked until it appears in a toxicology report. The drug that flies under standard drug screens also flies under most surveillance systems, which means the true scale of gabapentin dependency in Canada is larger than any current figure reflects.
Catching dependency early, before it compounds with other substances or reaches high doses, remains the most effective intervention available.
FAQ
Is gabapentin a controlled substance in Canada?
Gabapentin is not federally scheduled as a controlled substance in Canada, though several provinces have implemented prescription monitoring programmes due to rising misuse rates. Its legal status doesn't reflect its dependency potential, particularly for individuals with a history of substance use disorders.
Who is most at risk of developing gabapentin dependency?
People with a current or prior substance use disorder carry a markedly elevated risk. High-dose and long-term use increases dependency risk in anyone, but those combining gabapentin with opioids, alcohol, or benzodiazepines face the greatest danger.
Can quitting gabapentin cause seizures in someone without epilepsy?
Yes. Abrupt discontinuation of gabapentin has been documented to trigger seizures, including status epilepticus, in individuals with no prior seizure history. This risk is most pronounced with high-dose use and is why gradual tapering under medical supervision is non-negotiable.
What does gabapentin withdrawal feel like?
Physically, it resembles a severe case of the flu – sweating, palpitations, nausea, and muscle pain. The psychological symptoms, particularly anxiety and sleep disruption, are often worse and last longer. Gabapentin withdrawal can be delayed by up to a week after the last dose, so someone may feel fine for several days and assume the worst has passed, then get hit by the full syndrome.
How long does gabapentin withdrawal last?
Most people experience peak symptoms within the first week, with physical symptoms generally resolving within 5 to 10 days. Psychological symptoms, like mood instability, sleep disruption, and persistent low mood, may take several weeks to fully lift. The timeline depends on dosage, duration of use, and whether other substances are involved.





