We offer medical detox and multiple addiction treatment options in our
luxury treatment centres in Port Hope, Cobourg, and Ottawa.
Can You Force Someone Into Treatment?
Canadian law does not give families the right to admit an adult into rehab against their will. That's the reality most people hit when they start looking for options, and it's a hard one, especially when the person they're trying to help is clearly in danger.
What the law does allow is narrower and more conditional: a physician can authorize compelled addiction treatment, but only after an independent assessment confirms specific clinical grounds. Where you live, what the doctor finds, and what happens next all shape what's actually possible. Here's what the Mental Health Act permits in practice, and what your options look like when voluntary substance abuse treatment isn't on the table.
Key Takeaways:
- Why families have less legal authority than most assume – and which single professional holds the only power that actually matters under Canadian law.
- What a physician has to find before signing a Form 1, and why a loved one can be in serious decline without qualifying for an involuntary hold.
- How long an involuntary hold can last in Ontario – and what has to happen at each stage before detention can be extended further.
- Why your province of residence changes everything – including one jurisdiction where patients under an involuntary hold can be treated without their agreement.
- Where parental authority over a teenager's treatment actually ends – and at what age a young person can legally refuse addiction care regardless of what their parents want.
Can You Force Someone Into Rehab for Addiction in Canada?
No, not as an individual acting alone. Canadian law gives families no direct authority to admit an adult into compulsory care against their will. That power rests exclusively with a licensed physician, and only after a face-to-face assessment.

What families can do is create the conditions for a physician to act. Two practical routes exist.
The first: bring the person to a hospital emergency department. If the physician on duty concludes they meet the legal threshold for involuntary detention, admission can proceed without any family consent being required.
The second: call police under Section 17 of Ontario's psychiatric detention law, which authorizes officers to apprehend someone and transport them to a physician for assessment. If there are reasonable grounds to believe the person poses a danger to themselves or others.
Neither route guarantees admission. The physician makes the final call. And the criteria are specific, where substance abuse alone is not sufficient grounds. The addiction must be producing either demonstrable danger or a measurable, documented deterioration in physical or mental health. This is where many families run into difficulty – their loved one may be in serious decline without meeting the precise clinical thresholds the legislation requires. A structured intervention is often the more effective path before any legal route is even considered.
How Does the Mental Health Act Work in Practice?
The Mental Health Act in Canada is provincial legislation. Each province administers its own version, though the underlying criteria follow a broadly consistent pattern. There is no federal-level provision for compulsory detention; this is entirely a matter of provincial health law.
In Ontario, the Mental Health legislation outlines a specific form-based system that governs every involuntary admission. Only a physician can trigger an involuntary admission, and only after conducting an in-person assessment. No judge, family member, or police officer can compel psychiatric detention on their own – the decision must originate with medical authority.
A Danger to Themselves or Others
The clearest ground for involuntary alcohol rehab or drug-related detention is demonstrated danger. If a person's substance abuse has led them to threaten suicide, attempt self-harm, threaten another person, or take actions that create genuine risk to others, a physician can complete a Form 1, a Psychiatric Assessment certificate, authorizing up to 72 hours of involuntary admission to a psychiatric facility.
Police can also bring someone to a physician for assessment under the same Section 17 provision if they have reasonable grounds to believe the person is a danger to themselves or others. The officer does not admit the person; they bring them to a doctor, who then decides.
During those 72 hours, the treating physician assesses the patient. If the grounds for continued detention are confirmed, they can issue a Form 3 (Certificate of Involuntary Admission), which extends detention for up to two weeks. A Certificate of Renewal can extend this further, first by one month, then by two-month intervals, as long as the criteria continue to be met.
Deteriorating Condition
The second pathway applies when the person isn't posing an immediate threat, but their condition is clearly worsening. A physician who evaluates the individual and concludes that their addiction or mental health state has deteriorated to a point where hospitalization is medically necessary, even without acute danger, can also authorize an involuntary hold for an initial 72-hour period under the same Form 1 authority.

Even after admission, treatment itself cannot always be forced. Ontario's Health Care Consent Act draws a distinction between detention and treatment. A person who retains mental capacity can refuse specific medications or therapies, even when being held involuntarily. Forced treatment in the fullest sense only applies after capacity to consent has been formally assessed and found to be absent.
How Long Does Forced Treatment Last?
Initial detention under Ontario's involuntary commitment framework runs for 72 hours. From there:
- Form 3 (Certificate of Involuntary Admission): up to two additional weeks
- First Certificate of Renewal: up to one additional month
- Subsequent Renewals: up to two additional months each
There is no fixed upper ceiling written into the legislation, but each renewal requires a fresh physician assessment confirming that the criteria are still being met. The physician cannot simply extend detention as a matter of course; the patient's condition must continue to justify it.

How Do Provincial Laws on Forced Rehab Differ Across Canada?
Court-ordered addiction treatment and compulsory detention for drug dependence are governed differently depending on where you live.
📍Ontario applies the form-based detention system described in the previous section, with one distinction worth noting separately. Even after involuntary admission, a patient who retains mental capacity can refuse specific treatments. There is no deemed consent in Ontario, unlike in BC. A physician cannot compel someone to take methadone, buprenorphine, or any other medication if that person retains the capacity to decline. Involuntary alcohol rehab in Ontario amounts, in practice, to supervised stabilization rather than active addiction treatment. The person is held safely, but medication-assisted treatment still requires their agreement.
📍British Columbia operates under its own provincial mental health statute, which permits involuntary apprehension, assessment, and treatment. BC's legislation includes a "deemed consent" provision for people with involuntary status, meaning that, unlike Ontario, BC can compel certain treatments even when the patient objects. Initial detention is capped at 48 hours, but a second physician certificate can extend this for up to one month, renewable for three months, then six months. In March 2025, BC opened its first dedicated involuntary treatment facility in Surrey for justice-involved people who use drugs. BC also reports approximately 30,000 involuntary psychiatric apprehensions annually – the highest rate in the country.
📍Alberta is the most legislatively active province on this issue right now. In April 2025, the Alberta government tabled Bill 53, the Compassionate Intervention Act. If passed, it would allow family members, caregivers, healthcare professionals, and police officers to petition for a treatment order for adults whose addiction poses a danger to themselves or others. It makes the first dedicated adult addiction forced treatment statute in Canada.
📍Quebec and the Atlantic provinces operate under their own frameworks with varying thresholds and duration limits, but all follow the same core principle: involuntary treatment requires physician authorization and is time-limited.
Does Forced Rehab Apply to Minors in Canada?
The Mental Health Act applies to children as well as adults, and this creates an important distinction that many parents misunderstand. You cannot simply admit a child under 16 into involuntary alcohol rehab or drug treatment as a parent. The same physician-driven criteria apply: danger to self or others, or severe deteriorating condition, and a doctor must independently assess and authorize any involuntary admission.
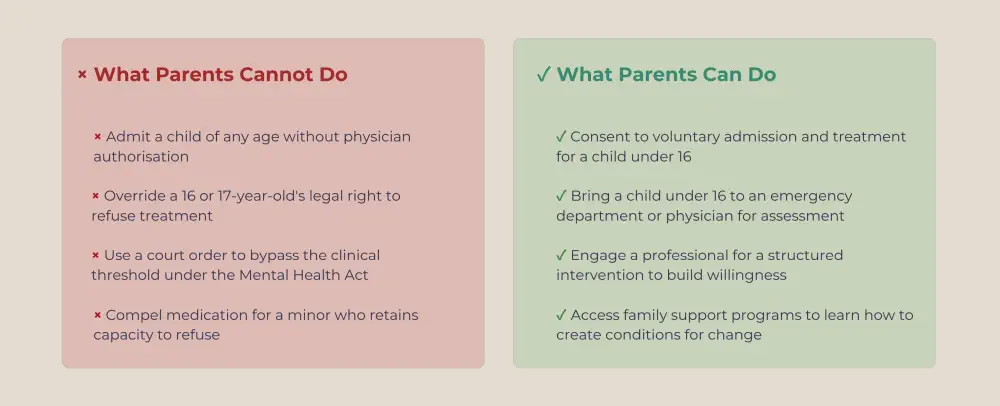
For children under 16, a parent or guardian can consent to voluntary admission and treatment on the child's behalf. Youth aged 16 and 17 are generally treated as having adult capacity to consent or refuse, which means they can legally decline addiction treatment even when a parent disagrees.
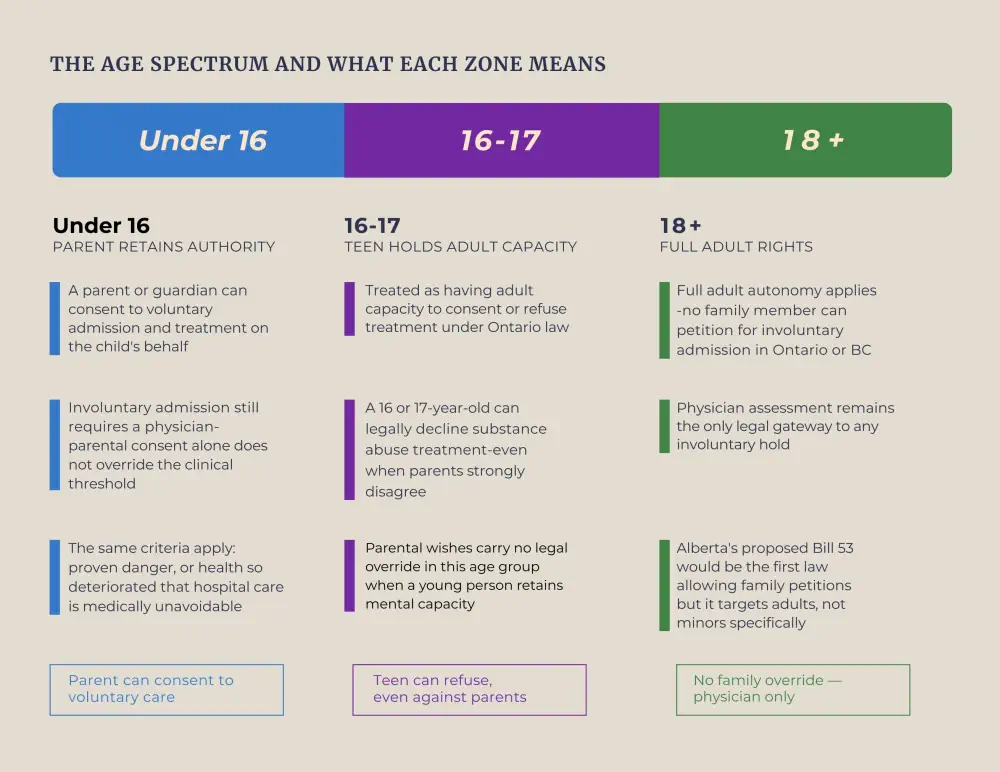
This is a painful reality for parents watching teenagers spiral. Help for an addicted loved one, minor or adult, begins not with legal force but with proper professional guidance on how to create the conditions for change.
What Alternatives to Forced Rehab Are Available?
Before pursuing any legal avenue, and in most cases, long before reaching that point, there are meaningful alternatives that produce better outcomes with less damage to the family relationship.
Professional intervention is the most evidence-supported option when someone refuses help. A structured intervention led by a trained specialist, not family members acting alone, creates a carefully prepared conversation where the consequences of continued addiction are made real and immediate. Done well, it moves the emotional dynamic from confrontation to compassion and gives the person a dignified path into treatment.
CRAFT (Community Reinforcement and Family Training) teaches family members specific behavioural skills to reduce enabling, communicate more effectively, and reinforce moments when the addicted person moves toward recovery. Unlike traditional interventions, CRAFT takes a longer view, one that works even when the person isn't yet ready to enter treatment.
Motivational interviewing delivered by a counsellor can gently surface the person's own reasons for wanting change, without the pressure that so reliably triggers resistance. Professional intervention counselling at the Canadian Centre for Addictions is specifically designed to help families prepare for these conversations with the right tools and the right support. Our programmes offer a continuum of care that makes the transition from intervention to treatment as seamless as possible, for people entering voluntarily and for those who need a structured period of professional guidance first.

What Happens to Drug Tolerance During an Involuntary Hold?
The period immediately following involuntary release carries a danger most families don't anticipate. During detention, a person's drug tolerance drops, sometimes dramatically. If they return to street drugs at their previous dose within days of discharge, the risk of fatal overdose climbs sharply. Research cited by CMHA BC notes that detention itself can increase overdose risk post-release precisely because of this tolerance collapse, particularly for people who use fentanyl.
This is not an argument against forced treatment in crisis situations. It is an argument for what must follow it. The involuntary period creates a window: detox occurs, acute danger is interrupted, and the person is medically stable. What determines if that window becomes a turning point is having medication-assisted substance abuse treatment and a genuine care plan in place before the person walks out the door. Discharge planning is not an afterthought; for this population, it is where outcomes are actually decided.
Families whose loved ones have completed an involuntary hold should immediately engage their care team about transition options. At the Canadian Centre for Addictions, our treatment programmes are designed to receive people at exactly this juncture. When the acute crisis has passed, but the real recovery work hasn't yet begun. Speak with our team at 1-855-499-9446 to understand your options before that discharge date arrives.
FAQ
Can a family member legally force an adult into rehab in Canada?
Not directly. Families can call police under Section 17 of the Mental Health Act or bring the person to a hospital emergency department. Both routes lead to a physician assessment. Admission, however, requires a doctor's judgment. The family initiates the path; the physician decides.
What is a Form 1 under the Ontario Mental Health Act?
A Form 1 is a Psychiatric Assessment certificate that a physician completes to authorize up to 72 hours of involuntary admission. It applies when substance abuse has produced a danger to the person or others, or when their condition has deteriorated to the point of requiring immediate hospitalization.
How long can someone be held in involuntary treatment in Canada?
In Ontario, the initial hold is 72 hours. A physician can extend this to two weeks, then one month, then two-month intervals, each requiring a fresh assessment. Every extension must be clinically justified, not automatically renewed.
Does involuntary rehab actually work?
Outcomes depend on the type of treatment provided. Abstinence-based models in involuntary settings show no improvement over no treatment at all for opioid use disorder. Medication-assisted treatment, buprenorphine or methadone, does show measurable reductions in overdose risk.
What can I do if my loved one refuses help but isn't in immediate danger?
A professionally facilitated intervention is the most effective next step. Voluntary substance abuse treatment, entered when the person is ready, produces far stronger long-term outcomes than involuntary alcohol rehab. Call us at 1-855-499-9446 to discuss your options.
Article sources
- Government of Ontario (2024). "Mental Health Act, R.S.O. 1990, c. M.7." Ontario Laws. Available at: https://www.ontario.ca/laws/statute/90m07
- Canadian Society of Addiction Medicine Task Force (2023). "Involuntary Treatment for Substance Use Disorders: A Systematic Review." Canadian Journal of Addiction. Available at: https://journals.lww.com/cja
- CMHA Ontario (2024). "Involuntary Treatment: Provincial and Territorial Overview." Canadian Mental Health Association Ontario. Available at: https://ontario.cmha.ca/involuntary-treatment/
- Werb, D., et al. (2020). "The Effectiveness of Compulsory Drug Treatment: A Systematic Review." International Journal of Drug Policy. Available at: https://pubmed.ncbi.nlm.nih.gov
- CBC News (2024). "Forcing people into drug treatment is on the political agenda. Here's what the evidence says." CBC News. Available at: https://www.cbc.ca/news/health/involuntary-addiction-treatment-research-evidence-1.7377257
- Healthy Debate (2024). "Involuntary drug treatment: 'Compassionate intervention' or policy dead end?" Healthy Debate. Available at: https://healthydebate.ca/2024/06/topic/involuntary-drug-treatment-compassionate-intervention-policy-dead-end/
- Government of British Columbia (2025). "Mental Health Act." BC Laws. Available at: https://www.bclaws.gov.bc.ca/civix/document/id/complete/statreg/96288_01





